Women who have had to undergo surgery for breast cancer can experience emotional healing with breast reconstruction. Using different surgical approaches, breast reconstruction can reconstruct one or both breast masses and nipples after they have been surgically removed. Below are the two main approaches to breast reconstruction and the candidates best suited for each type.
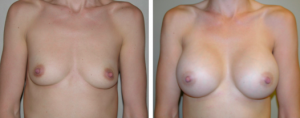
Autologous Reconstruction
For autologous reconstruction, the doctor will harvest tissue from either your abdomen or your back, and this tissue will be used to rebuild the breast mound. This approach includes the more commonly referred to “TRAM” flap procedure, in which abdominal skin and fat are harvested, and the “lat” flap procedure, in which the latissimus back muscle tissue is harvested. The tissue is extracted and then moved to the chest, where it is reshaped and reattached to recreate the appearance of the breast mound. This tissue provides a good substitute that can look and feel quite natural in place of the breast, and results will usually last a lifetime.
Ideal Candidates for Autologous Reconstruction
Ideal candidates for autologous breast reconstruction will be in good health after their mastectomy. Autologous reconstruction is best suited for those who have undergone a single mastectomy rather than a double mastectomy because the reconstructed breast tissue will mature like natural breast tissue. Candidates will need to have enough excess tissue to extract for this breast reconstruction approach. For women who have undergone a single mastectomy and whose remaining healthy breast is large, autologous reconstruction may not be able to harvest sufficient tissue to achieve breast symmetry. In this case, autologous reconstruction may be combined with implant reconstruction, or a breast reduction can be performed on the healthy breast to achieve symmetry.
Implant Reconstruction With Tissue Expander
The implant reconstruction with tissue expander approach is performed in two stages. In stage one, a tissue expander or temporary breast implant device is placed in the breast pocket after the mastectomy. This tissue expander helps to prepare the skin and tissues to hold a future permanent breast implant. Stage two is usually performed about four to six months after stage one and replaces the tissue expander with a permanent breast implant. With this technique, the implant or implants may need to be replaced at some point in the future. The breast implant reconstruction with tissue expander approach may also require alteration of the healthy breast in order to achieve symmetry. Recovery and length of surgery are usually shorter with this approach than with autologous reconstruction, as only the chest area is surgically altered.
Ideal Candidates for Implant Reconstruction With Tissue Expander
Ideal candidates for implant reconstruction with tissue expander will not need radiation therapy for their breast cancer treatment. This approach is best suited for patients who must undergo a double mastectomy. This procedure avoids creating incisions in other areas of the body and is appropriate for those who want or need an easier or shorter recovery experience with breast reconstruction. Dr. Oliver and Dr. Jack are both well experienced and trained in performing each of these surgical techniques for breast reconstruction. When you come in for your consultation, the doctor will go over your medical history and recommend the treatment that he feels is best for you and your needs. In many cases, breast reconstruction will be conducted in multiple stages in order to achieve the best results. With breast reconstruction, you can receive the closure and emotional healing you need after overcoming breast cancer.
To learn more about breast reconstruction after mastectomy, contact our office to schedule your consultation with one of our board-certified plastic surgeons, Dr. Robert I. Oliver, Jr. or Dr. Jason M. Jack. Please call (205) 298-8660 or fill out our online contact form to schedule your appointment today.
